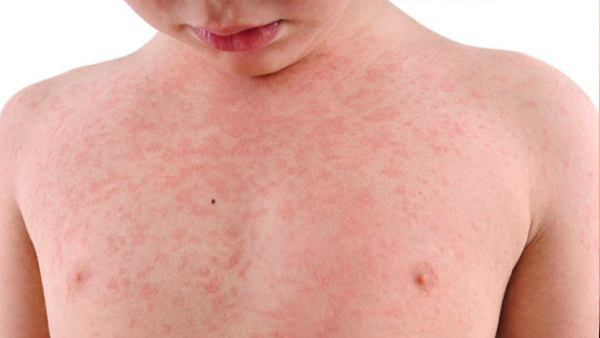
Skin Rash in Children: Complete Diagnosis and Treatment Guide for Parents in Dubai
Skin rashes are among the most common reasons parents bring their children to see a pediatrician. From mild irritations that resolve on their own to signs of serious allergic reactions requiring immediate attention, skin rashes in children can be concerning and confusing for parents. At myPediaClinic in Dubai Healthcare City, Dr. Medhat Abu-Shaaban and our pediatric team regularly diagnose and treat various skin conditions in children, helping families understand what’s causing their child’s rash and how to address it effectively.
This comprehensive guide explores the many causes of skin rashes in children, how different types of rashes are diagnosed, when to seek medical attention, and what treatments are most effective for various conditions affecting children in Dubai and the UAE.
Understanding Skin Rashes in Children
A skin rash is any change in the skin’s color, texture, or appearance. Rashes can appear as red patches, raised bumps, blisters, welts, or scaly areas. They may be localized to one area of the body or spread across multiple regions. Understanding the characteristics of your child’s rash helps healthcare providers determine the underlying cause and appropriate treatment.
Why Children Are Prone to Skin Rashes
Children’s skin is more sensitive and reactive than adult skin. Their immune systems are still developing, making them more susceptible to infections and allergic reactions. Children also have more frequent skin-to-skin contact with others, share objects that may carry irritants or infectious agents, and often encounter new substances their bodies have never experienced before. These factors combine to make skin rashes a common occurrence throughout childhood.
Common Causes of Skin Rashes in Children
Skin rashes in children can result from numerous causes, ranging from harmless viral infections to serious allergic reactions. Identifying the cause is essential for proper treatment and preventing complications.
Allergic Reactions
Allergies are among the most frequent causes of skin rashes in children. Allergic rashes occur when the immune system overreacts to a substance it perceives as harmful, even though that substance may be completely harmless to most people.
Food Allergies
Common food allergens that cause skin reactions in children include milk, eggs, peanuts, tree nuts, wheat, soy, fish, and shellfish. Food allergy rashes typically appear as hives (raised, itchy welts) but may also cause eczema flares or generalized redness and swelling. These reactions usually develop within minutes to two hours after eating the trigger food.
Medication Allergies
Antibiotics, pain relievers like aspirin and ibuprofen, and other medications can trigger allergic skin reactions. Drug allergy rashes may appear as hives, red patches, or more severe reactions involving skin peeling or blistering. Any new medication should be monitored carefully, and parents should report skin changes to their healthcare provider immediately.
Insect Bites and Stings
Mosquito bites are extremely common in Dubai and can cause significant allergic reactions in some children. As Dr. Medhat Abu-Shaaban has observed in clinical practice, a single mosquito bite can trigger an allergic response that spreads beyond the bite location, causing rashes in multiple body areas. This type of reaction, while alarming to parents, is typically manageable with appropriate treatment.
Contact Dermatitis
Direct skin contact with allergens or irritants causes contact dermatitis. Common culprits include certain metals (nickel in jewelry), fragrances in soaps and lotions, laundry detergents, plants, and latex. The rash appears where the skin touched the offending substance, often with clear boundaries matching the contact area.
Viral Infections
Many childhood viral infections cause characteristic skin rashes. These rashes are often accompanied by fever, fatigue, and other symptoms of illness.
Roseola
Common in children between six months and three years of age, roseola typically begins with high fever lasting three to five days. When the fever breaks, a pink, spotty rash appears on the trunk and spreads outward. The rash is not itchy and resolves within a few days without treatment.
Fifth Disease
Caused by parvovirus B19, fifth disease produces a distinctive “slapped cheek” appearance with bright red rashes on both cheeks. A lacy, pink rash may also appear on the arms, legs, and trunk. By the time the rash appears, children are usually no longer contagious.
Hand, Foot, and Mouth Disease
This viral infection causes painful sores in the mouth and a rash of flat red spots or small blisters on the palms of the hands, soles of the feet, and sometimes the buttocks. Common in children under five, it spreads easily in childcare settings and schools.
Measles
Although vaccination has made measles rare, it still occurs. The measles rash begins on the face and spreads downward, consisting of flat red spots that may merge together. High fever, cough, runny nose, and red eyes typically precede the rash by several days.
Chickenpox
Chickenpox causes an itchy rash of red spots that progress to fluid-filled blisters, then crust over. New spots continue appearing for several days, so lesions in various stages are present simultaneously. While vaccination has reduced chickenpox significantly, breakthrough cases can still occur.
Bacterial Infections
Bacterial skin infections require antibiotic treatment and can become serious if not addressed promptly.
Impetigo
This highly contagious bacterial infection causes red sores that quickly rupture, ooze fluid, and develop honey-colored crusts. It commonly appears around the nose and mouth and spreads easily through direct contact or contaminated objects.
Cellulitis
A deeper bacterial skin infection, cellulitis causes an area of spreading redness, warmth, swelling, and tenderness. It requires prompt antibiotic treatment to prevent the infection from spreading to deeper tissues or the bloodstream.
Scarlet Fever
Associated with strep throat, scarlet fever produces a rough, sandpaper-like rash that typically starts on the neck and chest before spreading. The skin in body creases may become deeper red. Treatment with antibiotics is essential to prevent complications.
Skin Conditions
Eczema (Atopic Dermatitis)
Eczema is one of the most common childhood skin conditions, affecting up to 20% of children. It causes dry, itchy, red patches that may weep, crust, and thicken with scratching. Eczema tends to run in families and is associated with allergies and asthma. The condition is chronic but can be managed effectively with proper skincare and treatment.
Psoriasis
Less common in children than eczema, psoriasis causes thick, red, scaly patches covered with silvery scales. It most often appears on the scalp, elbows, knees, and lower back. Psoriasis is a chronic condition that tends to flare and remit throughout life.
Heat Rash
Common in Dubai’s hot climate, heat rash occurs when sweat ducts become blocked, trapping perspiration under the skin. It appears as tiny red bumps or clear blisters, often in skin folds, on the neck, chest, or areas covered by clothing. Keeping skin cool and dry typically resolves heat rash quickly.
Other Causes
Hives (Urticaria)
Hives are raised, itchy welts that can appear anywhere on the body. They may be triggered by allergies, infections, physical factors like cold or pressure, or have no identifiable cause. Individual hives typically last less than 24 hours, though new ones may continue appearing for days or weeks.
Ringworm
Despite its name, ringworm is a fungal infection, not a worm. It causes circular, red, scaly patches with clearer centers, giving a ring-like appearance. Ringworm is contagious and commonly affects the scalp, body, or feet (athlete’s foot) in children.
Diagnosing Skin Rashes in Children
Accurate diagnosis is essential for effective treatment. When you bring your child to myPediaClinic for a skin rash evaluation, our pediatric team uses a systematic approach to identify the cause.
Medical History
The diagnostic process begins with a thorough history. We ask about when the rash first appeared, whether it has spread or changed, associated symptoms like fever or itching, recent exposures to new foods, medications, or substances, similar rashes in family members or contacts, and the child’s medical history and allergies.
Physical Examination
Careful examination of the rash provides valuable diagnostic information. We assess the rash’s appearance (color, texture, shape of individual lesions), distribution pattern, whether lesions are raised or flat, presence of blisters, crusting, or scaling, and signs of scratching or secondary infection.
Diagnostic Tests
While many rashes can be diagnosed clinically, some require additional testing. Allergy testing can identify specific triggers for allergic rashes. Skin scraping and microscopic examination help diagnose fungal infections. Bacterial cultures determine the best antibiotic for infected rashes. Blood tests may be needed to evaluate for systemic conditions.
Treatment Approaches for Common Childhood Rashes
Treatment depends on the underlying cause and severity of the rash. Many mild rashes resolve with simple home care, while others require medical treatment.
Managing Allergic Rashes
For allergic reactions, identifying and avoiding the trigger is paramount. Antihistamines relieve itching and reduce hive formation. Topical corticosteroids decrease inflammation for contact dermatitis and localized allergic rashes. Severe allergic reactions involving breathing difficulty, facial swelling, or rapid symptom progression require immediate emergency care and may necessitate epinephrine (EpiPen) administration.
Treating Infectious Rashes
Viral rashes typically require only supportive care—rest, fluids, fever reducers, and time for the infection to run its course. Bacterial infections need antibiotic treatment, either topical for localized infections like impetigo or oral for more extensive infections. Fungal infections respond to antifungal creams or, for resistant cases, oral antifungal medications.
Managing Eczema
Eczema management focuses on maintaining skin hydration, reducing inflammation, and preventing flares. Key strategies include daily bathing followed by immediate moisturizer application, using fragrance-free products, applying prescription topical medications during flares, identifying and avoiding individual triggers, and keeping nails short to minimize scratching damage.
Heat Rash Treatment
For heat rash, cooling the skin is the primary treatment. Move to air-conditioned environments, remove excess clothing, and allow skin to air dry. Cool baths may help, and calamine lotion can soothe affected areas. Preventing heat rash by dressing children in loose, breathable clothing is preferable to treating it after it develops.
When to Seek Medical Attention
While many childhood rashes are harmless, certain signs warrant prompt medical evaluation. Contact a healthcare provider when your child has a rash accompanied by high or persistent fever, a rash that spreads rapidly, blistering or open sores, signs of infection such as increasing redness, warmth, swelling, or pus, a rash that doesn’t improve with home treatment after several days, or significant pain or discomfort.
Seek emergency care immediately if your child has a rash with difficulty breathing, facial or throat swelling, severe weakness or lethargy, purple or blood-colored spots that don’t fade when pressed, or signs of meningitis including stiff neck, severe headache, and sensitivity to light.
Preventing Skin Rashes in Children
While not all rashes are preventable, certain measures reduce risk and minimize recurrence.
Skincare Basics
Use gentle, fragrance-free soaps and detergents. Moisturize regularly, especially after bathing. Avoid excessive bathing that strips natural skin oils. Dress children in soft, breathable fabrics and avoid known skin irritants.
Allergy Prevention
For children with known allergies, strict avoidance of triggers prevents reactions. Read food labels carefully, inform caregivers and schools of allergies, and carry emergency medication as prescribed. For children at risk of severe allergic reactions, ensure they wear medical alert identification.
Infection Prevention
Teach children proper hand hygiene. Keep vaccinations up to date to prevent vaccine-preventable rash-causing illnesses. Don’t share towels, combs, or personal items with others. Treat any skin infections promptly to prevent spread.
Managing Dubai’s Climate
The hot, humid climate in Dubai increases risk for heat rash and certain infections. Dress children appropriately for the weather, ensure adequate hydration, and provide access to cool environments during extreme heat. Use appropriate sun protection to prevent sunburn.
The Importance of Professional Evaluation
While many parents attempt to diagnose and treat their child’s rash at home using internet resources, professional evaluation offers significant advantages. Pediatricians can distinguish between conditions that look similar but require different treatments. We can identify signs of serious illness that require prompt intervention. We provide treatment plans tailored to your child’s specific situation. And we can establish whether a rash is contagious and advise on returning to school or childcare.
At myPediaClinic in Dubai Healthcare City, our pediatric team is experienced in diagnosing and managing all types of childhood skin conditions. We understand that a rash on your child can be worrying, and we’re committed to providing prompt, thorough evaluation and effective treatment.
Frequently Asked Questions About Childhood Skin Rashes
How do I know if my child’s rash is serious?
Certain features suggest a rash may be serious and needs medical evaluation. Be concerned if the rash is accompanied by high fever, appears as purple or blood-colored spots that don’t blanch (fade) when pressed, spreads rapidly, involves blistering or skin peeling, is associated with difficulty breathing or swallowing, or if your child appears very unwell. When in doubt, it’s always better to have a healthcare provider evaluate the rash rather than wait and see.
Can a single mosquito bite cause a rash in other areas of the body?
Yes, this is more common than many parents realize. Some children develop allergic reactions to mosquito bites that extend beyond the bite site. The immune response can cause hives, swelling, or generalized rash in areas distant from where the actual bite occurred. This happens because the allergic reaction triggers a systemic response, releasing histamine and other chemicals that affect skin throughout the body. These reactions, while alarming, typically respond well to antihistamines and generally aren’t dangerous unless breathing is affected.
When can my child return to school after having a rash?
This depends entirely on what’s causing the rash. Rashes from allergic reactions, eczema, heat rash, and most viral infections after the fever has resolved are not contagious, and children can attend school if they feel well enough. Bacterial infections like impetigo require 24 hours of antibiotic treatment before returning. Chickenpox requires all lesions to be crusted over. Ringworm needs 24 hours of antifungal treatment. Hand, foot, and mouth disease policies vary, but children often can return once fever-free without fever-reducing medication. Your pediatrician can advise on the specific situation.
How can I tell the difference between eczema and an allergic reaction?
Eczema and allergic rashes can look similar but have distinguishing features. Eczema typically affects characteristic locations (face in infants, skin folds in older children), causes dry, thickened skin, and has a chronic, recurring pattern. Allergic rashes like hives appear suddenly, may be associated with a specific trigger, and individual lesions typically resolve within 24 hours. Allergic contact dermatitis has clear boundaries matching where the skin contacted the allergen. Your pediatrician can help differentiate between these conditions and recommend appropriate treatment.
My child has recurring hives but we can’t identify a trigger. What should we do?
Chronic hives (lasting more than six weeks) often have no identifiable cause, which can be frustrating for families. Keep a detailed diary of your child’s diet, activities, exposures, and hive episodes to look for patterns. Allergy testing may help identify triggers, though it often doesn’t reveal a cause in chronic hives. Management focuses on controlling symptoms with daily antihistamines while waiting for the condition to resolve on its own, which it typically does within months to a few years. Consult with a pediatric allergist if hives are severe or not responding to standard treatment.
Is it safe to use over-the-counter hydrocortisone cream on my child’s rash?
Over-the-counter hydrocortisone (1% strength) is generally safe for short-term use on most childhood rashes to relieve itching and inflammation. However, it should not be used on the face, groin, or skin folds without medical guidance. It’s not appropriate for infectious rashes like ringworm (it can worsen fungal infections), impetigo, or viral rashes. Don’t use it for more than a week without consulting your pediatrician. If the rash isn’t improving or is worsening with hydrocortisone, stop use and seek medical evaluation.
What’s the best way to relieve my child’s itching from a rash?
Several strategies help relieve itching. Cool compresses or cool baths provide immediate relief. Moisturizers, especially when refrigerated, soothe itchy skin. Oral antihistamines like cetirizine or diphenhydramine reduce itching from allergic rashes. Keep nails short to minimize damage from scratching. Distraction with activities can help children resist the urge to scratch. Covering the rash with soft clothing prevents direct scratching. Topical hydrocortisone or other prescribed creams reduce inflammation that causes itching. Avoid hot water, harsh soaps, and tight clothing that can worsen itching.
Should I be worried about a rash that appears after starting a new antibiotic?
Rashes occurring during antibiotic treatment require careful evaluation. Many rashes during antibiotic use are actually caused by the underlying viral infection, not the antibiotic. However, true drug allergy rashes do occur and can range from mild to severe. Contact your pediatrician if your child develops a rash while on antibiotics. Seek emergency care immediately if the rash is accompanied by difficulty breathing, facial swelling, widespread blistering, or peeling skin. Never restart an antibiotic that previously caused a reaction without medical guidance.
Why does my child keep getting the same rash over and over?
Recurring rashes suggest either a chronic skin condition like eczema, ongoing exposure to an allergen or irritant, a condition with recurring episodes like psoriasis, or environmental factors that repeatedly trigger reactions. Identifying patterns helps determine the cause. Note when rashes occur, what preceded them, what makes them better or worse, and whether seasons or locations affect them. This information helps your pediatrician identify triggers and develop a prevention plan. For eczema and other chronic conditions, consistent daily skincare reduces flare frequency and severity.
Can weather changes or Dubai’s climate cause skin rashes in children?
Absolutely. Dubai’s hot, humid climate can trigger several types of rashes. Heat rash occurs when sweat ducts become blocked. Humidity promotes fungal infections like ringworm. Intense sun exposure causes sunburn. Air conditioning creates dry indoor environments that worsen eczema. The transition between extremely hot outdoor temperatures and cold air conditioning can stress the skin. Dust and sand can irritate sensitive skin. To minimize climate-related rashes, dress children in breathable fabrics, ensure adequate hydration, use appropriate sun protection, moisturize regularly, and allow gradual temperature transitions when possible.