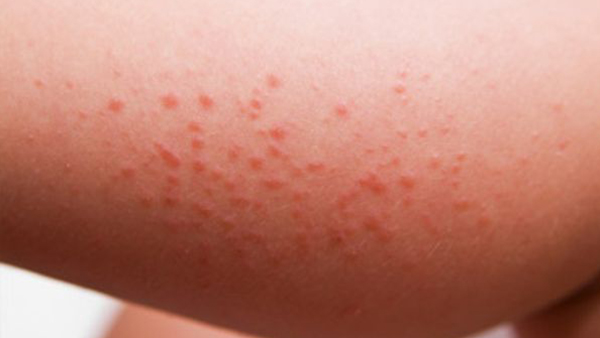
Skin Allergic Rash in Children: Complete Guide for Parents in Dubai
Has your child suddenly developed an itchy, red rash that seems to appear out of nowhere? Are you worried about the bumps, hives, or irritated patches on your little one’s skin? Skin allergic rashes are one of the most common reasons parents bring their children to see a pediatrician, and understanding what causes these reactions can help you protect your child and know when to seek medical attention.
Allergic skin reactions in children can range from mild, temporary irritations to more severe conditions that require ongoing management. The good news is that with proper identification of triggers and appropriate treatment, most children with skin allergies can live comfortably and enjoy normal activities. In Dubai’s unique environment, where children are exposed to various climatic conditions, indoor environments with air conditioning, and diverse products, understanding skin allergies becomes even more essential for parents.
At myPediaClinic in Dubai Healthcare City, our experienced pediatricians, including Dr. Medhat Abu-Shaaban, regularly diagnose and treat skin allergic rashes in children of all ages. This comprehensive guide explains the most common causes of allergic skin reactions in children and what you can do to help your child.
What Is an Allergic Skin Rash?
An allergic skin rash occurs when your child’s immune system overreacts to a substance that is normally harmless. The immune system mistakenly identifies this substance (called an allergen) as a threat and releases chemicals, including histamine, that cause inflammation and the characteristic symptoms of an allergic reaction. This process, known as hypersensitivity, can manifest in different ways depending on the type of allergen, the route of exposure, and your child’s individual immune response.
The skin serves as our body’s first line of defense against the external environment, and when the immune system perceives a threat—even a harmless one—it mobilizes various defensive mechanisms that unfortunately cause the uncomfortable symptoms we associate with allergic rashes.
How Allergic Reactions Develop
Understanding the process helps explain why some children develop allergies while others don’t:
- Sensitization: The first exposure to an allergen “sensitizes” the immune system, creating antibodies called Immunoglobulin E (IgE). During this phase, your child may not show any symptoms, but the immune system is “learning” to recognize the substance.
- Recognition: On subsequent exposures, the immune system recognizes the allergen through the previously created IgE antibodies attached to mast cells throughout the body.
- Reaction: The immune system releases histamine and other chemicals from mast cells, causing the cascade of symptoms we recognize as an allergic reaction.
- Inflammation: Blood vessels dilate and fluid leaks into tissues, causing redness, swelling, and warmth at the affected site.
- Itching: Nerve endings are stimulated by histamine and other inflammatory mediators, causing the characteristic itch that makes allergic rashes so uncomfortable for children.
- Resolution: Once the allergen is removed and inflammatory chemicals are broken down, symptoms gradually subside, though this can take hours to days depending on the severity.
Why Children Are More Susceptible
Children’s skin is more vulnerable to allergic reactions for several reasons:
- Thinner skin: Children’s skin is approximately 20-30% thinner than adult skin, making it more permeable to allergens and irritants that can penetrate the outer protective layer.
- Developing immune system: The immune system is still learning to distinguish true threats from harmless substances. This “learning period” can result in inappropriate reactions to benign substances.
- More frequent exposures: Children encounter many substances for the first time during early childhood, increasing opportunities for sensitization.
- Skin barrier immaturity: The protective skin barrier, including the stratum corneum and the skin’s natural oils, is still developing in children, allowing easier penetration of potential allergens.
- Higher surface area to body weight ratio: Children have greater relative skin surface area compared to their body weight, resulting in proportionally greater exposure to environmental factors.
- Frequent hand-to-face contact: Young children touch their faces frequently after touching various surfaces, transferring potential allergens directly to sensitive facial skin.
- Crawling and floor contact: Babies and toddlers spend significant time on floors where dust, pet dander, and other allergens accumulate.
Common Types of Allergic Skin Rashes in Children
Atopic Dermatitis (Eczema)
The most common chronic skin condition in children, affecting up to 20% of children worldwide:
- Appearance: Red, dry, itchy, scaly patches that may weep or crust when scratched
- Common locations: Face and scalp in infants; neck, elbows, knees, wrists, and ankles in older children
- Age of onset: Often begins in infancy (first 6 months), with approximately 85% of cases appearing before age 5
- Triggers: Dry skin, irritants, allergens, heat, humidity changes, stress, infections
- Associated conditions: Often occurs with asthma and hay fever (the “atopic triad”), suggesting a genetic predisposition to allergic conditions
- Course: Often improves with age but may persist or recur throughout life; approximately 50% of children outgrow eczema by adolescence
- The itch-scratch cycle: Intense itching leads to scratching, which damages the skin barrier, worsens inflammation, and increases itching—a cycle that must be actively broken
- Skin barrier dysfunction: Research shows that many children with eczema have mutations in the filaggrin gene, which is essential for skin barrier function
Contact Dermatitis
Develops when skin touches an allergen or irritant and comes in two main forms:
- Allergic contact dermatitis: A true immune reaction to specific substances such as nickel, fragrances, latex, certain plants, and preservatives in cosmetics. Requires prior sensitization.
- Irritant contact dermatitis: Direct skin damage from harsh substances such as soaps, detergents, acids, and alkalis. Does not require previous exposure—anyone can develop it with sufficient exposure.
- Appearance: Red, itchy, sometimes blistered rash typically appearing in the pattern of contact with the offending substance
- Timing: Allergic type appears 24-72 hours after exposure; irritant type is more immediate, sometimes developing within hours
- Common triggers in children: Costume jewelry (nickel), cosmetics and fragrances, rubber in shoes or clothing, adhesive bandages, certain plants (poison ivy, oak, sumac), hair dyes, and preservatives in skincare products
- Shoe dermatitis: A specific form common in children, caused by chemicals in rubber, dyes, or adhesives in footwear
- Diaper dermatitis: While often irritant-based, it can have allergic components related to fragrances in wipes or diapers
Urticaria (Hives)
Raised, itchy welts that appear suddenly and can be alarming for parents:
- Appearance: Raised, red or skin-colored welts (wheals) of varying sizes, often with pale centers and red borders
- Characteristic feature: Individual hives come and go within 24 hours, but new ones may appear in different locations, giving the impression of a “moving” rash
- Triggers: Foods, medications, viral infections (very common in children), insect stings, heat, cold, pressure, exercise, and sometimes emotional stress
- Acute hives: Last less than 6 weeks, often caused by identifiable triggers such as food allergies, viral infections, or medication reactions
- Chronic hives: Last more than 6 weeks; cause is often unknown (idiopathic) and may require ongoing management
- Dermographism: A physical form of hives where scratching or pressure causes welts to appear along the path of contact—literally “writing on the skin”
- Viral-induced hives: Extremely common in children; many viral infections trigger widespread hives that resolve as the infection clears
Angioedema
Deeper swelling beneath the skin that often occurs alongside hives:
- Appearance: Swelling of deeper skin layers, commonly affecting lips, eyelids, hands, feet, tongue, or genitals
- Characteristics: Less itchy than hives but may be painful, burning, or cause a sensation of tightness
- Often accompanies hives: About 40% of hives cases include angioedema; only 10% of patients have angioedema alone
- Duration: Takes longer to resolve than hives—typically 24-72 hours
- Concern: Swelling of throat, tongue, or airway structures requires immediate emergency medical attention as it can obstruct breathing
- Hereditary angioedema: A rare genetic condition that causes recurrent episodes unrelated to allergies, requiring specialized treatment
Papular Urticaria
A common childhood condition often confused with other rashes:
- Cause: Hypersensitivity reaction to insect bites, particularly from mosquitoes, fleas, bedbugs, or mites
- Appearance: Clusters of itchy, raised bumps that may persist for days to weeks
- Pattern: Often appears in groups on exposed areas, may recur seasonally
- Course: Children typically outgrow the hypersensitivity over several years of repeated exposure
Common Causes and Triggers of Skin Allergies
Food Allergies
Foods are a common cause of allergic skin reactions in children, particularly in the first years of life:
- Most common culprits: Cow’s milk, eggs, peanuts, tree nuts, wheat, soy, fish, and shellfish account for approximately 90% of food allergies in children
- Symptoms: Hives, itching, facial swelling, eczema flares, and in severe cases, anaphylaxis
- Timing: IgE-mediated reactions usually occur within minutes to 2 hours of eating
- Cross-reactivity: Allergies to one food may cause reactions to related foods (e.g., tree nut allergies often cross-react)
- Oral allergy syndrome: Children with pollen allergies may experience itching and mild swelling of lips and mouth when eating certain raw fruits and vegetables
- Non-IgE food allergies: Some food allergies cause delayed reactions (hours to days), making identification challenging
- Food protein-induced enterocolitis syndrome (FPIES): A severe non-IgE food allergy that can cause vomiting, diarrhea, and skin symptoms in infants
Environmental Allergens
Airborne and environmental substances can trigger or worsen skin reactions:
- Dust mites: Microscopic creatures living in household dust are a major trigger for eczema flares; their droppings contain allergenic proteins
- Pet dander: Proteins from animal skin, saliva, and urine cause reactions; cat allergens are particularly potent and can persist in environments for months
- Pollen: Seasonal pollens from trees, grasses, and weeds can worsen eczema during allergy seasons
- Mold: Both indoor and outdoor mold spores can trigger skin reactions in sensitive children
- Cockroach allergens: Common in urban environments, cockroach droppings and body parts are significant allergens
- Air pollution: Studies show that children exposed to higher levels of air pollution have increased rates of eczema
- Climate factors: Low humidity, extreme temperatures, and sudden weather changes can trigger flares in sensitive children
Contact Allergens
Substances that cause reactions when touching the skin directly:
- Nickel: The most common contact allergen worldwide, found in jewelry, belt buckles, zippers, buttons, electronics, eyeglass frames, and coins
- Fragrances: Found in perfumes, soaps, lotions, detergents, and even “unscented” products that may contain masking fragrances
- Preservatives: Chemicals like methylisothiazolinone, formaldehyde releasers, and parabens in cosmetics and personal care products
- Latex: Found in gloves, balloons, rubber bands, elastic in clothing, and some medical devices
- Plants: Poison ivy, poison oak, and poison sumac contain urushiol oil; other plants like chrysanthemums can also cause reactions
- Dyes: Textile dyes, especially dark colors and paraphenylenediamine (PPD) in hair dyes
- Topical antibiotics: Neomycin and bacitracin are common causes of allergic contact dermatitis
- Sunscreens: Certain chemical sunscreen ingredients can cause contact allergies in some children
Medications
Some medications can cause allergic skin reactions ranging from mild to severe:
- Antibiotics: Penicillin, amoxicillin, and related drugs are common culprits; sulfa antibiotics also frequently cause reactions
- NSAIDs: Ibuprofen and aspirin can trigger hives and angioedema in sensitive individuals
- Anticonvulsants: Some seizure medications, particularly phenytoin and carbamazepine, can cause severe skin reactions
- Viral illness interactions: Certain medications (like amoxicillin) combined with viral infections (like Epstein-Barr virus) can trigger dramatic rashes
- Reactions can range from: Mild maculopapular rash to severe, life-threatening reactions like Stevens-Johnson syndrome or drug reaction with eosinophilia and systemic symptoms (DRESS)
- Timing varies: Immediate reactions (within hours) versus delayed reactions (days to weeks after starting medication)
Insect Stings and Bites
Common cause of localized and sometimes systemic reactions:
- Bees, wasps, hornets: Venom can cause severe allergic reactions, including anaphylaxis in sensitized children
- Mosquitoes: Cause local reactions; some children develop Skeeter Syndrome with large, prolonged swelling
- Fire ants: Can cause pustules, significant local reactions, and occasionally systemic allergic reactions
- Fleas and bedbugs: Often cause papular urticaria with clusters of itchy bumps
- Sand flies: Common in the UAE and Middle East, can cause significant local reactions
Infections
Viral and bacterial infections can trigger skin reactions that may be confused with allergies:
- Viral infections: Many viruses cause hives in children; the rash may appear during or after the infection
- Strep throat: Can trigger scarlet fever rash or post-streptococcal reactive arthritis with skin manifestations
- Post-infectious rashes: Rashes may appear as the infection resolves, sometimes weeks later
- Gianotti-Crosti syndrome: A viral-triggered rash causing bumps on cheeks, buttocks, and extremities
Symptoms of Allergic Skin Reactions
Mild to Moderate Symptoms
- Redness and inflammation (erythema)
- Itching (pruritus) ranging from mild to intense
- Dry, scaly, or flaky skin
- Small bumps, papules, or vesicles (tiny blisters)
- Swelling at the affected area (localized edema)
- Hives (raised welts) that may change location
- Skin warmth at affected sites
- Skin thickening (lichenification) with chronic scratching
- Weeping or oozing from affected areas
- Crusting as weeping areas dry
Severe Symptoms Requiring Immediate Attention
Seek emergency care immediately if your child experiences:
- Difficulty breathing: Wheezing, shortness of breath, throat tightness, or stridor (high-pitched breathing sound)
- Swelling of face, lips, tongue, or throat: Risk of airway obstruction; this is a medical emergency
- Dizziness or fainting: Signs of anaphylaxis with cardiovascular involvement
- Rapid heartbeat: Tachycardia indicating systemic reaction
- Widespread hives: Spreading rapidly across the body
- Vomiting or diarrhea: Along with skin symptoms, suggesting systemic allergic reaction
- Confusion or altered consciousness: Indicating severe anaphylaxis
- Bluish coloring: Around lips or fingernails (cyanosis) indicating oxygen deprivation
Diagnosing Skin Allergies in Children
At myPediaClinic Dubai, our diagnostic approach is thorough and child-friendly:
Medical History
A detailed history is often the most valuable diagnostic tool:
- Detailed description of symptoms, their appearance, pattern, and distribution
- Timing of reactions relative to possible exposures
- Family history of allergies, eczema, asthma, or hay fever
- Diet and recent food exposures, including new foods introduced
- New products or environmental changes in the home
- Current medications and any recent medication changes
- Recent illnesses or infections
- Activities before symptom onset
- Impact on sleep, school, and daily activities
- Previous treatments and their effectiveness
Physical Examination
- Careful examination of the rash pattern, distribution, and characteristics
- Assessment of morphology (what the individual lesions look like)
- Evaluation of overall skin condition, including barrier function
- Checking for signs of secondary bacterial infection
- Examination for other allergic conditions (allergic rhinitis, asthma signs)
- Assessment of lymph nodes
- General health evaluation
Allergy Testing
When indicated, testing may include:
- Skin prick testing: Small amounts of allergens applied to the skin with a tiny prick; results visible in 15-20 minutes. Generally safe and well-tolerated by children.
- Blood tests (specific IgE): Measures antibodies to specific allergens; useful when skin testing isn’t possible or when the child is on antihistamines
- Patch testing: For contact dermatitis, allergens applied under patches for 48 hours then evaluated at 48 and 96 hours
- Elimination diets: Removing and systematically reintroducing suspected food allergens under medical supervision
- Oral food challenges: The gold standard for food allergy diagnosis, performed under medical supervision
- Component-resolved diagnostics: Advanced blood tests that identify specific allergenic proteins, helping predict reaction severity
Differential Diagnosis
Your pediatrician will also consider other conditions that can mimic allergic rashes:
- Viral exanthems (rashes caused by viral infections)
- Bacterial skin infections (impetigo, cellulitis)
- Fungal infections (ringworm, yeast)
- Scabies and other parasitic infections
- Psoriasis
- Seborrheic dermatitis
- Heat rash (miliaria)
Treatment Options for Allergic Skin Rashes
Avoidance of Triggers
The most important treatment is avoiding known triggers:
- Identify and eliminate specific allergens from your child’s environment
- Read product labels carefully for known allergens and irritants
- Inform schools, caregivers, relatives, and family friends about your child’s allergies
- Create an allergen-free environment at home when possible
- Develop an allergen management plan for travel and outings
- Keep a symptom diary to identify patterns and potential triggers
Topical Treatments
- Emollients and moisturizers: Essential for maintaining skin barrier function, especially for eczema. Apply liberally and frequently—at least twice daily and immediately after bathing. Choose fragrance-free, hypoallergenic products. Ointments are generally more effective than creams for very dry skin.
- Topical corticosteroids: Reduce inflammation effectively; various strengths available from mild (hydrocortisone 1%) to potent formulations. Use as directed by your pediatrician to minimize side effects.
- Topical calcineurin inhibitors: Non-steroid options (tacrolimus, pimecrolimus) for sensitive areas like face and skin folds, and for long-term use
- Anti-itch creams: Containing menthol, pramoxine, or other soothing ingredients for symptomatic relief
- Wet wrap therapy: For severe eczema, applying medication under wet bandages can enhance absorption and healing
- Topical PDE4 inhibitors: Newer medications (crisaborole) that reduce inflammation without steroids
Oral Medications
- Antihistamines: Block histamine to reduce itching and hives. Non-sedating options (cetirizine, loratadine, fexofenadine) are preferred for daytime use; sedating antihistamines (diphenhydramine) may help with sleep.
- Oral corticosteroids: For severe flares, short-term use can quickly reduce inflammation; not for long-term use due to side effects
- Antibiotics: If secondary bacterial infection develops, which is common when scratching breaks the skin
- Antiviral medications: If eczema herpeticum (herpes infection of eczematous skin) develops
- Biologics: For severe, refractory atopic dermatitis, newer injectable medications (dupilumab) may be considered in older children
Emergency Treatment
- Epinephrine (EpiPen/Auvi-Q): For children at risk of anaphylaxis; parents and caregivers must be trained in proper use
- Emergency action plan: Written plan detailing signs of severe reaction and steps to take, including when to use epinephrine and call emergency services
- Medical alert identification: Bracelet or necklace indicating severe allergies
Prevention and Management Strategies
Skin Care Basics
- Moisturize regularly: Apply fragrance-free moisturizer at least twice daily, more often for dry skin. The best time is immediately after bathing while skin is still slightly damp.
- Gentle bathing: Lukewarm (not hot) water, short baths (5-10 minutes), and mild, fragrance-free cleansers. Avoid bubble baths.
- Pat dry: Don’t rub skin after bathing; gently pat with a soft towel
- Apply moisturizer immediately: Within 3 minutes of bathing to lock in moisture (“soak and seal”)
- Avoid over-bathing: Daily baths may be too drying for some children; every other day may be sufficient
- Consider bleach baths: Dilute bleach baths (1/4 to 1/2 cup bleach in a full bathtub) can reduce bacterial colonization in children with frequent skin infections
Environmental Control
- Use hypoallergenic products: Fragrance-free soaps, detergents, and lotions for the whole family
- Wash new clothes: Before wearing to remove manufacturing chemicals and formaldehyde finishes
- Control dust mites: Use allergen-proof bedding covers for mattress, pillows, and comforters; wash bedding weekly in hot water (at least 130°F/54°C)
- Maintain optimal humidity: 30-50% indoor humidity; use humidifiers in dry seasons and air conditioning in humid weather
- Keep pets out of bedrooms: If pet allergies are suspected; consider keeping pets outdoors or in designated areas
- Regular cleaning: Vacuum with HEPA filter, damp dust surfaces, minimize carpeting and upholstered furniture in the child’s bedroom
- Air purifiers: HEPA air purifiers can reduce airborne allergens in the bedroom
- Avoid smoking: Tobacco smoke worsens eczema and overall allergy burden
Clothing Choices
- Choose soft, breathable fabrics (100% cotton is often best)
- Avoid wool and synthetic materials directly against skin
- Remove tags that may irritate
- Dress in layers to prevent overheating
- Wash clothes with hypoallergenic detergent and rinse thoroughly
- Avoid fabric softeners and dryer sheets, which can leave irritating residue
- Consider specialized eczema clothing made from silk or specialized fabrics
Managing Itch
- Keep fingernails short and smooth to minimize scratching damage
- Consider cotton gloves or mittens at night for young children
- Use cold compresses to soothe itchy areas
- Teach older children distraction techniques when they feel the urge to scratch
- Maintain cool room temperatures, especially at night
When to See a Pediatrician
Consult myPediaClinic Dubai if your child has:
- A rash that doesn’t improve with home care after one week
- Signs of infection (pus, increasing redness, red streaks, fever)
- Severe itching that disrupts sleep or daily activities
- Recurrent rashes without known cause
- Rash accompanied by other symptoms (fever, joint pain, fatigue)
- Any signs of severe allergic reaction (breathing difficulty, facial swelling)
- Skin condition affecting your child’s quality of life or emotional well-being
- Need for prescription treatments or specialist referral
- Interest in allergy testing to identify specific triggers
Long-Term Management and Prognosis
Living with Chronic Skin Allergies
For children with chronic conditions like eczema:
- Develop a daily routine: Consistent skin care becomes second nature over time
- Learn to recognize flares early: Early treatment prevents severe episodes
- Work with your healthcare team: Regular follow-ups help optimize treatment
- Address emotional impacts: Chronic skin conditions can affect self-esteem and mental health
- Prepare for school: Communicate with teachers about your child’s needs
- Build a support network: Connect with other families managing similar conditions
Outgrowing Allergies
Many children outgrow certain allergies:
- Eczema often improves significantly by adolescence
- Milk, egg, wheat, and soy allergies are often outgrown by school age
- Peanut, tree nut, fish, and shellfish allergies are more likely to persist
- Regular monitoring by your pediatrician can track allergy status over time
Expert Care at myPediaClinic Dubai
At myPediaClinic in Dubai Healthcare City, we provide comprehensive care for children with skin allergies:
- Accurate diagnosis of skin conditions using the latest diagnostic approaches
- Allergy testing when indicated, with child-friendly techniques
- Personalized treatment plans tailored to your child’s specific needs
- Parent education on trigger avoidance and skin care techniques
- Management of chronic conditions like eczema with evidence-based protocols
- Emergency action plans for children with severe allergies
- Coordination with allergists and dermatologists when specialist care is needed
- Support for families navigating the challenges of childhood allergies
Dr. Medhat Abu-Shaaban and our pediatric team have extensive experience helping children with allergic skin conditions live comfortably and confidently. We understand the impact these conditions have on the whole family and are committed to providing compassionate, comprehensive care.
Frequently Asked Questions
What causes allergic skin rashes in children?
Allergic skin rashes occur when the immune system overreacts to normally harmless substances. Common causes include food allergies (milk, eggs, peanuts, tree nuts), contact with irritants (soaps, detergents, nickel), environmental allergens (dust mites, pet dander, pollen), insect bites, and certain medications. Some children have genetic predisposition to allergies, especially if parents have allergies, asthma, or eczema. The immune system becomes sensitized to these substances and releases histamine and other chemicals that cause inflammation, redness, and itching whenever exposure occurs.
How can I tell if my child’s rash is allergic or something else?
Allergic rashes typically appear shortly after exposure to a trigger, are very itchy, and may include hives (raised welts) or eczema-like patches. They often recur with repeated exposures to the same trigger. Non-allergic rashes may be caused by viral infections (often with fever), bacterial infections (may have pus or spreading redness), fungal infections (ring-shaped patches), or other conditions like heat rash. The pattern, timing, and associated symptoms help differentiate causes. If you’re unsure, consult a pediatrician who can examine the rash and determine the cause through careful evaluation.
When should I take my child to the doctor for a skin rash?
Seek immediate medical care if your child has difficulty breathing, facial or throat swelling, or signs of anaphylaxis such as dizziness, rapid heartbeat, or confusion. Schedule a doctor visit if the rash is severe, spreading rapidly, shows signs of infection (pus, increasing redness, fever, red streaks), doesn’t improve with home treatment after a few days, causes significant discomfort affecting sleep or daily activities, or if you’re unsure of the cause. Also seek care if your child seems unwell beyond just the skin symptoms or if the rash recurs frequently without explanation.
Can food allergies cause skin rashes in children?
Yes, food allergies are a common cause of skin rashes in children. IgE-mediated reactions typically occur within minutes to two hours after eating the trigger food. Common symptoms include hives (raised, itchy welts), facial swelling, and eczema flares. The most common food allergens in children are cow’s milk, eggs, peanuts, tree nuts, wheat, soy, fish, and shellfish. Some food allergies cause delayed reactions affecting the skin hours to days later. If you suspect a food allergy, keep a detailed food diary noting what your child eats and when symptoms appear, then consult your pediatrician for proper evaluation and testing.
How can I relieve my child’s itchy allergic rash at home?
To relieve itching, apply cool compresses to affected areas for 10-15 minutes several times daily. Use fragrance-free moisturizers liberally and frequently. Give age-appropriate antihistamines as directed by your pediatrician. Keep fingernails trimmed short to prevent scratching damage. Dress your child in loose, soft cotton clothing. Maintain a cool room temperature, especially at night when itching often worsens. Colloidal oatmeal baths can soothe irritated skin. Avoid known triggers, harsh soaps, and hot water. For persistent symptoms, over-the-counter hydrocortisone cream may help, but consult your doctor for proper guidance.
Will my child outgrow their skin allergies?
Many children do outgrow certain allergies. Food allergies to milk, egg, wheat, and soy are often outgrown by school age, with about 80% of children with these allergies becoming tolerant over time. Eczema often improves significantly by adolescence, though some children continue to have sensitive skin. However, allergies to peanuts, tree nuts, fish, and shellfish are more likely to persist into adulthood—only about 20% of peanut-allergic children outgrow the allergy. Regular follow-up with your pediatrician can help monitor your child’s allergy status over time through periodic testing and supervised challenges when appropriate.
What is the difference between eczema and hives?
Eczema (atopic dermatitis) causes chronic, dry, itchy, scaly patches that tend to occur in specific locations (face in infants, elbows and knees in older children) and persist over time with periods of flare-ups and improvement. The skin often becomes thickened with chronic scratching. Hives (urticaria) are raised, red or skin-colored welts that appear suddenly, are very itchy, and typically come and go within hours—individual hives lasting less than 24 hours but new ones appearing elsewhere. Hives can appear anywhere on the body and are often triggered by specific allergens, infections, or medications. Eczema requires ongoing skin care management, while hives typically resolve once the trigger is removed.
Can laundry detergent cause skin rashes in children?
Yes, laundry detergents, especially those with fragrances, dyes, or harsh chemicals, can cause irritant or allergic contact dermatitis in sensitive children. The rash typically appears where clothing contacts skin, often on the trunk, waist, or areas where clothing fits snugly. To prevent reactions, use fragrance-free, dye-free, hypoallergenic detergents labeled for sensitive skin. Run an extra rinse cycle to remove all detergent residue. Avoid fabric softeners and dryer sheets, which can leave irritating residue on fabrics. Wash new clothes before wearing to remove manufacturing chemicals. If reactions persist, consider specialized detergents designed for eczema-prone skin.
Should my child with skin allergies see an allergist?
Consider seeing an allergist if your child has severe or frequent allergic reactions, if triggers cannot be identified despite careful observation, if standard treatments aren’t providing adequate relief, if your child has multiple allergies affecting quality of life, if there’s concern about anaphylaxis risk, or if you want comprehensive allergy testing to identify specific triggers. An allergist can perform specialized testing, develop detailed management plans, and consider treatments like immunotherapy when appropriate. Your pediatrician can provide a referral and help coordinate care with the allergist for optimal management of your child’s condition.
Are allergic skin rashes contagious?
No, allergic skin rashes like eczema, hives, and contact dermatitis are not contagious. They result from your child’s immune system reacting to allergens and cannot be spread to others through touch or close contact. However, if eczema becomes infected with bacteria (impetigo) or viruses (eczema herpeticum), those secondary infections can be contagious. Viral rashes that may look similar to allergic rashes can also be contagious, so proper diagnosis is important. If you’re unsure whether your child’s rash is allergic or infectious, consult your pediatrician for proper evaluation and guidance on any precautions needed.
Can stress cause skin rashes in children?
While stress doesn’t directly cause allergic rashes, it can trigger or significantly worsen existing skin conditions like eczema and hives. Stress affects the immune system through the release of cortisol and other stress hormones, which can lower the threshold for allergic reactions and increase inflammation. Children under stress may also scratch more frequently and intensely, worsening their skin condition through the itch-scratch cycle. Managing stress through adequate sleep, regular physical activity, relaxation techniques, and addressing underlying emotional concerns can help improve skin symptoms. If you notice your child’s skin flares during stressful times, discuss stress management strategies with your pediatrician.
What should I do if my child has a severe allergic reaction?
For severe allergic reactions (anaphylaxis) with breathing difficulty, facial/throat swelling, dizziness, or rapid heartbeat: Call emergency services (998 in UAE) immediately. Use an epinephrine auto-injector (EpiPen/Auvi-Q) if prescribed—inject into the outer thigh and hold for 10 seconds. Lay your child flat with legs elevated (unless having breathing difficulty, then keep upright). Stay calm and monitor breathing while waiting for help. Even if symptoms improve after epinephrine, your child must be evaluated at a hospital as reactions can recur (biphasic reaction). Always have two epinephrine auto-injectors available and ensure all caregivers know how to use them.
How can I prevent allergic skin rashes in my child?
Prevention focuses on avoiding known triggers and maintaining healthy skin. Keep skin well-moisturized with fragrance-free products applied at least twice daily. Use gentle, hypoallergenic soaps and detergents. Dress your child in soft, breathable cotton clothing. Control environmental allergens like dust mites with allergen-proof bedding covers and regular cleaning. Identify and avoid food triggers confirmed through proper testing. Introduce new products one at a time so you can identify any that cause problems. Maintain optimal indoor humidity (30-50%). Avoid tobacco smoke exposure. Work with your pediatrician to develop a personalized prevention plan based on your child’s specific triggers.
For expert evaluation and treatment of your child’s skin allergies, visit myPediaClinic in Dubai Healthcare City. Schedule an appointment today with our experienced pediatric team led by Dr. Medhat Abu-Shaaban. We are committed to helping your child achieve healthy, comfortable skin and a better quality of life.